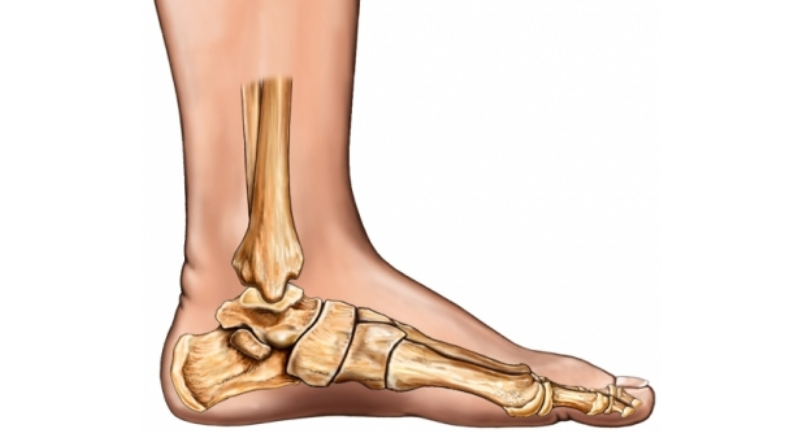
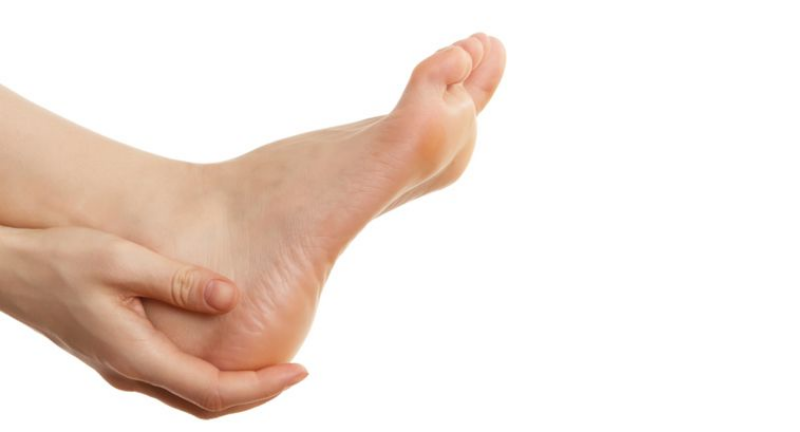
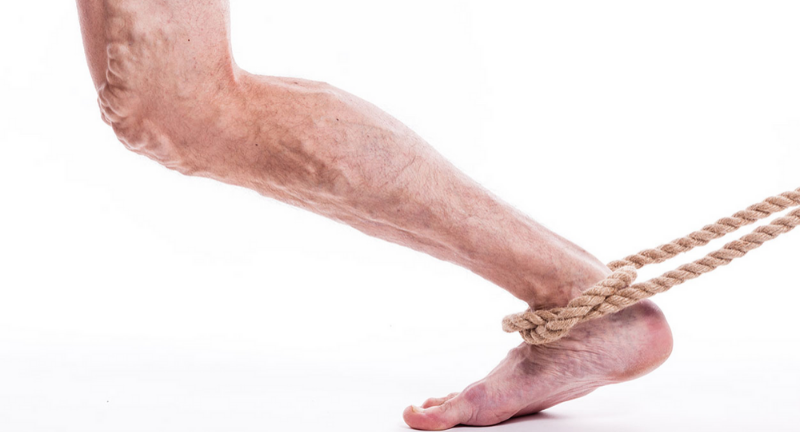
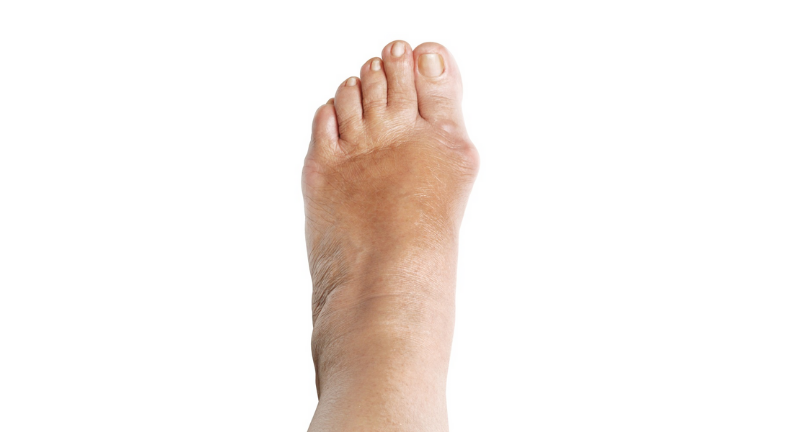
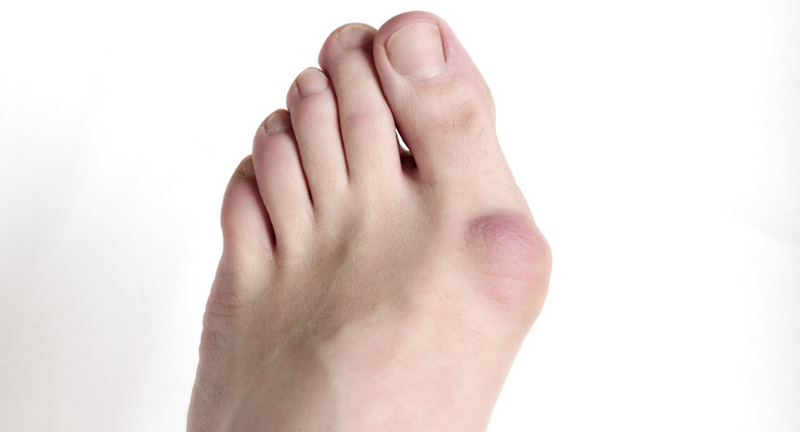
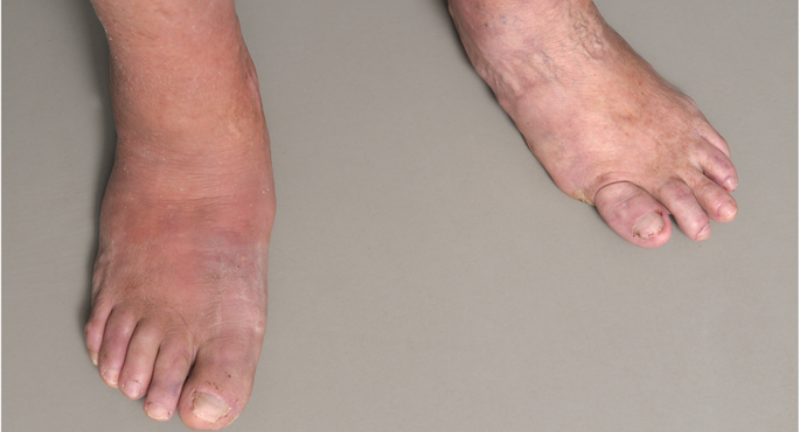
There are several possible causes for the limited range of ankle motion. Often it is due to tightness in the Achilles tendon or calf muscles (the soleus muscle and /or gastrocnemius muscle). In some patients, this tightness is congenital and is sometimes an inherited trait. Other patients acquire the tightness through situations that keep the foot pointing downward for extended periods- such as being in a cast, being on crutches or frequently wearing high heeled shoes. In addition, diabetes can affect the fibers of the Achilles tendon and cause tightness.